What Is Dental Billing? A Guide to How Dental Billing Works in 2026
17 Mar 2026 By: Mary Dellosa
Updated

Dental billing is the process dental offices use to charge patients and insurance companies for services, from verifying coverage to submitting claims and collecting payments. It ensures the practice gets paid accurately and on time. For example, after a filling, the office codes the procedure, sends a claim to insurance, and bills the patient for any remaining balance like deductibles or copays.
Let’s be honest: dental billing is usually the invisible leak in a successful practice. A single mistyped code can stall a payment for weeks, and an unverified insurance plan can turn a productive day into a major collection headache.
The ADA points out that these little hiccups actually add up to a loss of 5% to 10% in yearly revenue. To put that into perspective, if your practice brings in $800,000, you might be watching $80,000 walk right out the door. That is basically the cost of a high-end operatory setup or a new staff member lost simply because of paperwork friction.
The Fundamentals of Dental Billing
Defining the Dental Billing Cycle
Think of the dental billing cycle as the financial heartbeat of your office. It covers every single dollar that moves between your practice, your patients, and the insurance companies. It actually starts long before a patient even sits in the chair and it doesn’t really end until every penny is either in the bank or officially accounted for.
A typical cycle is a team effort that includes everything from that first registration call to verifying insurance, documenting the chairside work, and finally sending off the claim. Each step is like a domino. If you skip insurance verification, you’ll end up sending claims to the wrong place. If the treatment notes are a bit thin, you can expect a denial. If payments aren’t posted carefully, your accounts receivable becomes a giant headache that’s hard to untangle later on.
Most practices try to wrap up this entire process within 30 to 45 days. However, the top-performing offices usually have their money in hand within 21 days. The secret to moving that fast isn’t some hidden trick. It really just comes down to how well your team works together to keep things moving and how quickly you can catch a snag before it jams up the entire works.
Medical vs. Dental Billing Differences
It is a common mistake to think that dental and medical billing are the same thing, but mixing them up is a recipe for a headache.
For starters, the “languages” they speak are totally different. Medical billing uses one set of codes, while dental billing uses its own specific list from the ADA. Even the way claims are sent is different, since dental offices usually work with specialized systems or go straight to the insurance company.
The way the money works is the biggest surprise for most people. Medical insurance is designed to protect you from huge, scary bills once you hit a certain limit. Dental insurance is almost the opposite. It usually has a “cap” on how much it will pay out each year often just $1,000 or $2,000. Plus, the coverage changes depending on the work being done. Usually, the insurance handles 100% of a cleaning, 80% of a simple filling, and only 50% of something big like a crown.
The Step-by-Step Dental Billing Process
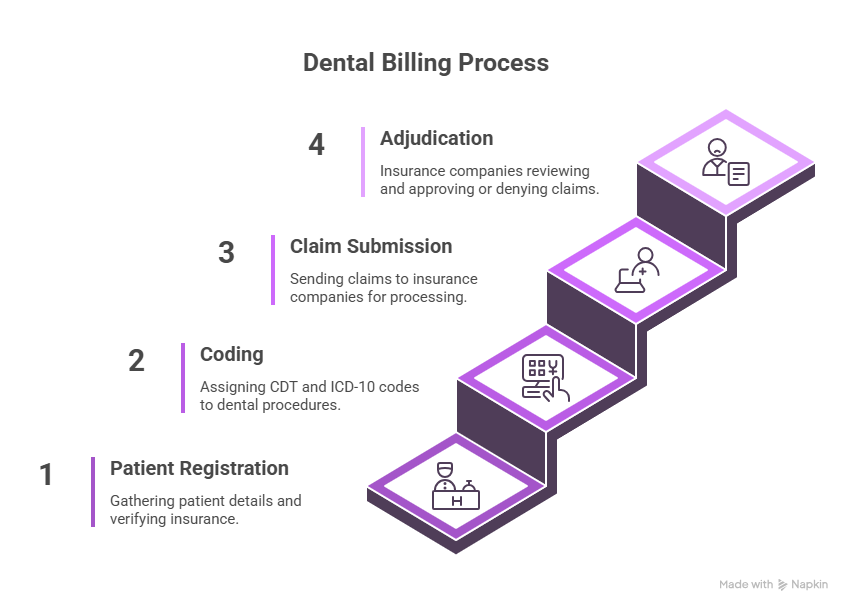
Patient Registration and Insurance Verification
Signing a patient in feels like a tiny task, but a small mistake here can mess up everything later. You need the right details, up-to-date insurance, and a solid handle on what their plan actually covers before any work starts.
Verifying insurance just means double-checking that the patient’s coverage is active and seeing what is left in their “bucket” for the year. The best offices do this at least two days before the appointment.
Doing this early lets you fix any issues or give the patient a heads-up before they arrive. It is really about the basics: is their insurance even active today? How much of their yearly limit is left? Do they have a deductible to pay first? You also want to check for “fine print” like how often they can get a cleaning or if there is a waiting period before they can get a crown.
Coding with CDT and ICD-10 Systems
Think of coding as the language your office uses to talk to insurance companies. You use CDT codes to explain exactly what happened in the chair, from a basic cleaning to a complex surgery. Picking the right one is a big deal because even a small typo can lead to a “denied” stamp or a smaller check than you earned.
Sometimes, you might even use medical codes. This is a lifesaver when dental work is tied to a health issue, like an extraction before radiation therapy. Getting these right can actually unlock medical benefits that a standard dental plan wouldn’t touch.
The most common blunders are usually simple mix-ups, like labeling a surgical extraction as a “simple” one or getting the number of surfaces on a filling wrong. Every little mistake like that either slows down your payment or leaves your hard-earned money on the table.
Claim Submission and Adjudication
Once the codes are locked in, the claim is ready to be sent to the insurance carrier in a process known as submission. Most modern offices do this electronically through a clearinghouse to avoid “snail mail” delays and catch simple errors instantly.
After the claim hits the insurer’s desk, it enters the adjudication phase. This is essentially the insurance company’s internal review where they double-check the patient’s eligibility, plan limits, and clinical necessity. If everything aligns, they approve the payment.
However, if they need more proof, such as an X-ray or a written narrative explaining why a crown was necessary, they will “pend” the claim. HelpSquad’s billing experts are trained to handle these pended claims immediately by gathering the right documentation, which is the best way to protect your cash flow and ensure that 21-day turnaround.
Managing Patient Collections and Payments
Calculating Copayments and Deductibles
“Patient responsibility” is just a fancy way of saying what the patient actually has to pay out of pocket. Getting this number right before the appointment is a game-changer. It helps patients plan their budget and makes it way more likely you’ll actually get paid.
Think of it like this: if a crown costs $1,200, but insurance only “approves” $1,000 of that price, the math starts there. After a $50 deductible, the plan pays half of what’s left, which leaves the patient with a $525 bill. If you aren’t in their network, they might also have to cover that extra $200 difference, bringing their total out-of-pocket to $725. Putting it in these terms helps patients see exactly where their money is going before the work even starts.
The secret to a healthy practice is asking for that payment the day they come in. If you wait to send a bill until after insurance pays, your chances of collecting that money drop to about 60%. If you collect it at the front desk before they leave, that number jumps to 95% or higher.
Handling Denied and Rejected Claims
Every office gets claims sent back. What sets the successful practices apart is how fast they jump on those “denied” stamps.
Usually, it is something simple:
- A typo in the patient’s name or ID number
- The insurance plan just doesn’t cover that specific treatment
- The patient already had that procedure too recently (like a cleaning)
- You forgot to get “permission” (prior authorization) first
- The insurance wants two codes combined into one
When a claim hits a wall, you have to be a bit of a detective. Was it just a quick clerical fix? Does the patient need to pay the balance instead? Or did the insurance company get it wrong and you need to push back?
If you notice the same code getting rejected over and over, that is a huge clue. It usually means there is a glitch in how you are writing your notes or how the claim is being filed. Catching those patterns early saves everyone a lot of time.
Essential Components of Successful Dental Billing
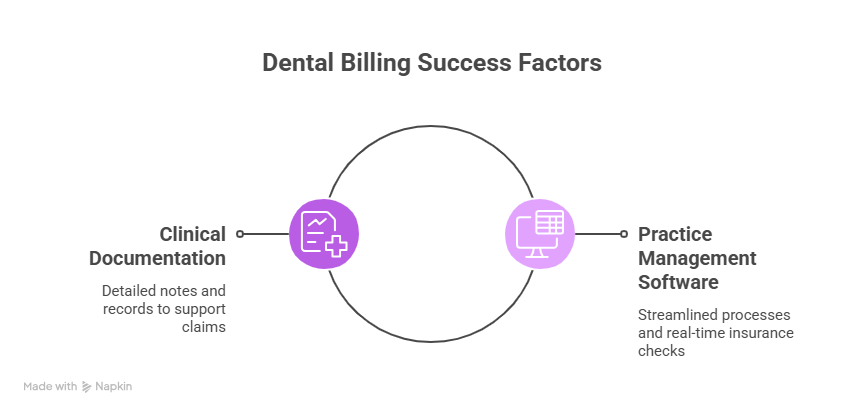
The Role of Proper Clinical Documentation
Your clinical notes are more than just a record of the visit. They are the proof you need to get paid. Think of them as your backup plan if an insurance company ever questions a bill. If your notes are too thin, a payer might try to take that money back or even flag your office for an audit.
The rule is simple: if you didn’t write it down, it never happened. Writing “prepped tooth for crown” usually isn’t enough to get paid. You need to show the “why” and “how” behind the work. Including clear X-rays, photos, and current gum charting makes a world of difference.
When you provide that kind of detail, it is much harder for an insurance company to say no. When you provide that kind of detail, it is much harder for an insurance company to say no to your claim.
Utilizing Dental Practice Management Software
Modern dental billing is just too fast for paper and spreadsheets. You need software that connects your schedule, patient charts, and dental billing in one place. If your system can’t talk to insurance companies in real time, you are likely working twice as hard for the same result.
A good system should do the heavy lifting for you. It should check if a patient is covered while they are on the phone, catch typos before you hit “send,” and show you exactly who owes you money. When your X-rays and notes are linked directly to the bill, the whole process feels much smoother.
This kind of setup pays for itself fast. You get your money sooner, deal with fewer “denied” stamps, and can finally see exactly how your practice is doing. It is all about catching those little glitches before they turn into expensive headaches.
In-House vs. Outsourced Dental Billing
Deciding whether to handle your dental billing in-house or hire an outside team is a big choice, and both ways can work great if they’re managed well.
Keeping it in-house means you have total control. Your team knows your patients personally and can chat with them directly about their bills. The catch is that you’re on the hook for hiring, training, and paying for their benefits and software.
Outsourcing hands those headaches to a company that lives and breathes dental claims. They have experts for every insurance quirk, and you don’t have to worry if someone calls in sick. In exchange, you lose a bit of direct control and usually pay a fee of 5% to 9% of what they collect for you.
Some offices find a middle ground that works best. You might keep the face-to-face patient payments in-house but let a specialist handle the messy insurance claims. It’s all about finding the right fit for your team’s rhythm.

Trending Now
Most people enter dentistry to help patients and build relationships, not to battle insurance companies. Unfortunately, the constant grind of confusing codes, claim denials, and frustrated patients can quickly “suck the fun” out of the job. This administrative stress doesn’t just stay at the front desk; it wears down the whole team, causes burnout, and hurts the practice’s bottom line. “Pushing through” often leads to more mistakes and higher turnover, but moving these heavy dental billing tasks to a dedicated partner allows your staff to finally focus on what they actually love: caring for people.
Conclusion
Mastering the dental billing cycle is vital for your practice’s health, but it shouldn’t come at the cost of team burnout or “paperwork friction.” Recognized as a Top Claims Processing Company for 2026 by Clutch, HelpSquad is a US-based BPO provider, delivering industry-leading support to dental practices nationwide.
Ready to plug the leaks in your revenue and get back to patient care? Talk to us today.
Frequently Asked Questions
1. Why does dental billing feel so much more stressful than clinical work?
Clinical work offers immediate results and closure, while billing is a never-ending cycle of paperwork. Between constantly changing insurance rules, confusing EOBs, and the mental load of chasing unpaid claims, billing can create a “constant uphill battle” feeling that clinical tasks simply don’t have.
2. How does billing stress affect the rest of my dental team?
Billing issues aren’t just a front-desk problem; they create a ripple effect. When the administrative team is burnt out, it can lead to friction with the clinical staff, slower patient check-ins, and a tense office atmosphere that patients can often sense, ultimately hurting your practice culture.
3. Can’t I just train my current staff to handle billing more efficiently?
While training helps, it often doesn’t solve the core issue. Insurance billing is increasingly complex and time-consuming. Piling more “efficiency” tasks onto an already busy team usually leads to faster burnout rather than better results. Sometimes the system, not the person, is what needs to change.
4. What are the signs that billing is “removing the fun” out of my practice?
Common red flags include high staff turnover in administrative roles, an increase in “bill shock” complaints from patients, and a growing list of claims that haven’t been touched in over 30 days. If your team spends more time on the phone with insurance than they do with patients, it’s a sign of a problem.
5. What is the biggest benefit of moving billing tasks off my team’s plate?
The biggest win is “mental freedom.” When experts handle the tedious follow-ups and appeals, your team can return to the parts of dentistry they actually enjoy like patient care and relationship building. This leads to a calmer office, happier patients, and more consistent cash flow.
Best Practices for Maximizing Practice Revenue
The best way to keep your practice healthy is to stop problems before they start. It’s all about a simple routine: check insurance before the patient arrives, collect their portion that day, and send the claim within 24 hours.
If you haven’t seen a check after 30 days, go ahead and give them a nudge. It is worth keeping an eye on how fast you’re getting paid and how many of your claims sail through on the first try. Most successful offices aim to get paid in under a month and have 95% of their claims accepted immediately.
Since insurance rules change every year, a little team training goes a long way. It’s also smart to “spot check” a few random claims now and then. You’ll often find tiny errors that are easy to fix before they become expensive headaches.
For practices finding that billing demands exceed their internal capacity, outsourcing to qualified professionals can transform financial performance. If you need support with billing tasks or other back-office operations, explore HelpSquad’s services for skilled assistance starting at $8.50 per hour. Their bilingual teams handle customer support and administrative work around the clock, letting your staff focus on patient care while collections stay on track.